How Early Detection Saves Lives
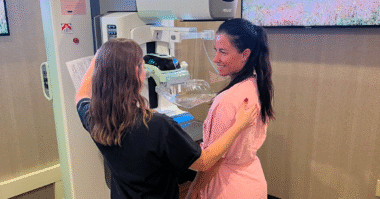
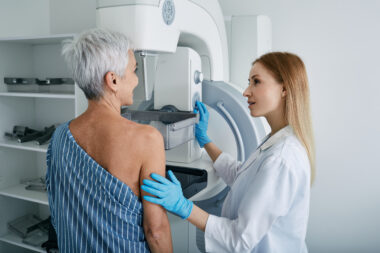
Meredith, a 52-year-old working mom, keeps up with healthy lifestyle habits, including maintaining a balanced diet and regular exercise. She faithfully schedules her annual wellness visit — including a screening mammogram — every 12 months, starting when she was 40.
During Meredith’s last annual screening mammogram, the radiologist found an area of concern that needed additional evaluation. Before this appointment, she had no prior breast health concerns and no family history of breast cancer and was considered at average risk for developing breast cancer. Diagnostic exams followed with additional imaging, including an ultrasound, a breast MRI, and two biopsies.
The results confirmed that Meredith had lobular carcinoma in situ (LCIS), characterized by abnormal cell growth in the milk glands of the breast. LCIS cannot be felt by touch and does not present with a lump, and it can only be detected through advanced imaging. According to the American Cancer Society, while not considered cancer, LCIS increases a woman’s risk for later developing invasive breast cancer in either breast. A patient with LCIS is considered high risk, requiring increased surveillance or screening every six months to catch even subtle changes in breast tissue that may develop into breast cancer.
Meredith’s LCIS developed during the year between her mammograms. Since you cannot detect LCIS with a self-exam, the condition would have gone undetected if Meredith hadn’t kept up with annual screenings. Instead, the area of concern was found early, removed, and is now being monitored.
“Now in my 50s, I am more ‘breast aware’ than ever before,” Meredith says.
“If not for my annual mammograms, I would have never known I was at higher risk for developing breast cancer. Now I screen every 6 months because I know early detection is so important, and I’ve made an even greater commitment to healthy diet and exercise”.
Read More: Breast Cancer Myths Debunked
Why an Annual Breast Screening Is Important
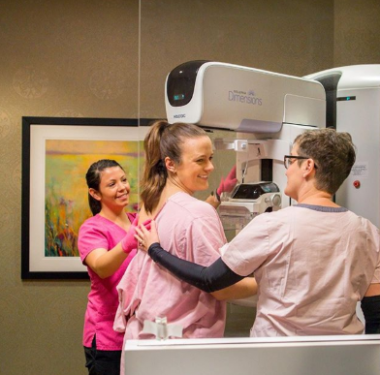 Meredith’s story demonstrates the power of keeping up with annual wellness visits. Even though she had no family history of breast cancer and led a healthy lifestyle, she still received an LCIS diagnosis. Since breast health changes over time, regular screening is the best tool to detect cancer or other areas of concern.
Meredith’s story demonstrates the power of keeping up with annual wellness visits. Even though she had no family history of breast cancer and led a healthy lifestyle, she still received an LCIS diagnosis. Since breast health changes over time, regular screening is the best tool to detect cancer or other areas of concern.
While some risk factors are related to genetics, the two biggest risk factors for breast cancer are being a woman and growing older. The Centers for Disease Control and Prevention estimates the average woman has a 1 in 8 risk for developing breast cancer, with most cases happening after age 50. Many women diagnosed with breast cancer have no known risk factors, and 3 out of 4 women diagnosed have no family history of the disease.
Breast cancer risk isn’t the only factor that changes with age. Your breasts themselves transform, with most changes happening around menopause — which typically happens between the ages of 45 and 55 — and with the natural decline of the female reproductive hormone estrogen. During this time, women experience changes in breast tissue and structure, with the breasts becoming smaller, fattier, and less firm or full. As dense breast tissue is replaced by fatty tissue, breast tissue becomes less uniform and the risk of growth — including fibroids, cysts, and cancer — increases. These growths can make it harder to determine what is cancerous and equally important, what is not.
That’s why an annual breast screening is so important. A 3D screening mammogram can identify even subtle changes in breast tissue, including early detection of breast cancers 2-3 years before a lump can be felt by a physician or patient. It can also help to identify changes that may indicate the presence of previously unknown risk factors, like LCIS or other changes that are non-cancerous that can be treated or managed, like cysts.
The goal of annual screening mammograms is to detect breast cancers early when they can be more effectively treated. Clinical experience has shown that detecting cancer at stages 0 or 1, the earliest stages, when diseased tissue is smaller and confined to the breast, can lead to less invasive treatment options and better outcomes with a five-year survival rate of nearly 100%. In fact, clinical data has demonstrated that annual screening mammograms starting at 40 years of age has reduced breast cancer deaths by approximately 40%.
Read More: Put Your Breast Health Knowledge to the Test
Breast Screening: A Key Part of Self-Care
You know your body and your health, and you take steps to nurture wellness and to try to control for risk factors for disease through preventive health practices. One such step is seeing your OB-GYN or primary care provider each year for a women’s wellness visit. Another is having an annual screening mammogram to check your breast health.
Your breast health changes year over year. And for women, the risk for developing breast cancer increases as we age which makes annual screening a vital wellness check. Identifying risk and finding breast cancers early through mammography leads to early diagnosis and treatment with a much better prognosis.
 Knowing the importance of regular mammograms isn’t always enough for women to prioritize self-care, especially when we are organizing activities for our families, putting in extra hours at work, or helping aging parents. Yet focusing on a healthier you, including breast health, ensures you can stay on top of your day-to-day ‘to do’ list, be there for the people you love, and be fully present and productive in your own pursuits both now and in the future. No matter how busy life gets as you grow older, remember you need to put self-care first. Like Meredith, sticking to a healthy diet, staying active with regular exercise, and prioritizing your breast health by staying on top of your annual well visits gives you the best prevention regimen possible.
Knowing the importance of regular mammograms isn’t always enough for women to prioritize self-care, especially when we are organizing activities for our families, putting in extra hours at work, or helping aging parents. Yet focusing on a healthier you, including breast health, ensures you can stay on top of your day-to-day ‘to do’ list, be there for the people you love, and be fully present and productive in your own pursuits both now and in the future. No matter how busy life gets as you grow older, remember you need to put self-care first. Like Meredith, sticking to a healthy diet, staying active with regular exercise, and prioritizing your breast health by staying on top of your annual well visits gives you the best prevention regimen possible.
Here are some steps you can take now to promote overall health and wellness — including breast health:
- Eat healthily. Combined with exercise, a diet rich in fruits, vegetables and whole grains — minimizing red meat, high-sugar and processed foods — can help you fuel your body with good nutrition and maintain a healthy weight. That’s important because being overweight or obese is a risk factor for breast cancer.
- Exercise regularly. Work toward a goal of completing at least 30 minutes of moderate-intensity exercise most days of the week. Clinical studies conducted over the past 20 years have consistently shown that regular increased physical activity is linked to lower breast cancer risk.
- Know your breasts. Be “breast aware” by keeping up with monthly self-breast exams and clinical exams at your annual well-woman visit. Report any concerns- including new lumps or thickening in the breast or armpit area, abnormal nipple changes or discharge, or changes in breast shape, size or skin (color, dimpling or puckering) to your primary care or OBGYN physician.
- Stay up to date with annual screening mammograms. Breast health experts and clinical guidelines recommend starting mammograms age 40 and continuing every year for women at average risk with no breast concerns. If you have known risk factors and/or a family history of breast, ovarian or other cancers, talk to your physician. He or she may suggest more frequent screenings (every six months compared to annual) or starting screenings earlier with a baseline screening at age 35.
Schedule Your Annual Screening Mammogram Today
Sources:
- Slide decks by Dr. Stephanie Morgan, Charlotte Radiology
- https://medlineplus.gov/ency/article/003999.htm
- https://www.cancer.gov/types/breast/breast-changes/dense-breasts
- https://www.cancer.gov/types/breast/breast-changes/understanding-breast-changes.pdf
- https://www.cdc.gov/cancer/breast/basic_info/screening.htm
- https://www.cancer.gov/types/breast/risk-fact-sheet
- https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/breast-cancer-facts-and-figures/breast-cancer-facts-and-figures-2019-2020.pdf
- https://seer.cancer.gov/statfacts/html/breast.html
- https://www.cdc.gov/cancer/breast/young_women/bringyourbrave/breast_cancer_young_women/index.htm
- https://www.sbi-online.org/endtheconfusion/PatientResources/WhyScreenat40.aspx
- https://gis.cdc.gov/Cancer/USCS/#/Demographics/
- https://www.cdc.gov/cancer/breast/basic_info/risk_factors.htm
- https://www.sbi-online.org/endtheconfusion/Blog/TabId/546/ArtMID/1586/ArticleID/467/What-Can-I-Do-to-Reduce-My-Odds-of-Being-Diagnosed-with-Breast-Cancer.aspx
- https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
- https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/stages-of-breast-cancer.html
- https://www.cancer.org/latest-news/five-ways-to-reduce-your-breast-cancer-risk.html