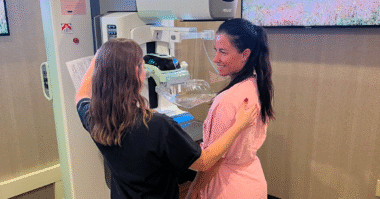
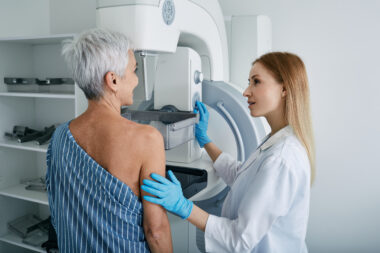
A new study from the Cancer Intervention and Surveillance Modeling Network (CISNET) reinforces the benefits of annual screening mammograms starting at age 40. The CISNET 2023 study findings emerge as a beacon of clarity in the ever-evolving landscape of breast health guidelines from health organizations like the National Comprehensive Cancer Network (NCCN) and the U.S. Preventive Services Task Force, which offer varying guidelines for breast cancer screening. The new CISNET study provides even more evidence to support the standard of care for “40 and annual” screening mammograms as a vital tool in detecting breast cancer early and saving more lives.
Read More: 4 Things to Know About the USPSTF New Draft Guidance for Mammograms
Who is CISNET?
The Cancer Intervention and Surveillance Modeling Network is a group of researchers who use data modeling to improve understanding of cancer control measures in prevention, screening and treatment and their effects on populations and survivorship. The group was established in 2000 by the National Cancer Institute, and they have since played an integral role in guiding public health research and recommendations for screening guidelines, including breast cancer screening guidelines.
The new CISNET 2023 study is the most recent and complete analysis confirming what many breast cancer guidelines recommend, adding to the growing body of evidence supporting annual screening starting at age 40 for women of average risk. This new data serves to inform breast cancer screening guidance across organizations so that it can be more consistent and uniformly adopted by patients and physicians, which is important because data shows that fewer than 50% of women screen annually.
The CISNET 2023 Study, Explained
The recent study used previously published data to create models related to breast cancer screening, estimating the risks and benefits of four different scenarios:
- Screening mammograms every two years from age 40 to 74
- Screening mammograms every two years from age 50 to 74
- Annual screening mammograms from age 40 to 74
- Annual screening mammograms from age 40 to 79
Each of these scenarios aligns with a recommendation for breast cancer screening from one or more health organizations. The goal of the CISNET 2023 study was to understand how breast cancer risks and benefits vary between each of these scenarios or recommendations. After applying the models, the team analyzed each scenario to understand how the screening recommendations could impact women’s lives.
The study estimated the following outcomes:
- Reduced breast cancer mortality and increased survivorship
- More life years gained
- Better detection in reducing both false positive screenings and unnecessary or negative findings on biopsies
Key Findings of the Study
According to the results of the study, the benefits of annual screening mammograms were greatest for women who started screening at age 40 and continued every year to age 79 as compared to women who started screening later at age 50 or screened only every other year. Specifically, women ages 40-79 who screened annually had more life-years added, improved survivorship and lower mortality, with breast cancer deaths reduced by 42%. By comparison, screening mammography every other year starting at age 50 only lowered mortality risk by 25% and screening every two years from age 40 decreased the risk by 30%.
The CISNET study results consistently showed the greatest benefits for annual screening mammograms beginning at age 40 and continuing through age 79 for women with an average risk of breast cancer. Getting yearly mammograms from 40 to 79 saved the most lives from breast cancer and added the most years to people’s lives. The results also showed breast cancer screening beginning at 40 and continuing through 79 led to the lowest risk of false positives and benign biopsies per every 1,000 women screened, thus demonstrating the benefits of early and annual screening outweigh the potential risks of being called back or biopsied unnecessarily.
Read More: Breast Cancer in Young Women: Risk Factors and Early Detection
The Role of Annual Screening Mammography Starting at Age 40
Annual 3D mammography has been clinically shown in studies to reduce breast cancer deaths in women by 40% and is one of the most effective ways to evaluate changes in breast health year over year. Annual screening can also help detect some breast cancers up to three years before a lump can be felt by a physician or patient during a breast exam. When breast cancer is detected at stage 0 or 1, women have nearly a 100% five-year survival rate.
Early breast cancer detection is made possible by annual screening, and in many cases, earlier diagnosis leads to less invasive treatment, lower costs for the patient and most importantly, more lives saved. The new CISNET study shows that women who start mammograms at 40 and return every year through age 79 have the best chance of early detection and breast cancer survival.
If you’re nearing or over 40, talk with your healthcare provider to learn more about breast cancer screening and what you can do to maintain and monitor your best breast health. For women at higher risk for developing breast cancer, screening mammograms may be started earlier in their 30s. And of course, if you have any breast health concerns like a lump or discharge, be sure to consult with your primary care physician or OBGYN to determine if imaging may be required. Your healthcare provider can help answer your questions about mammograms at any age, so start the dialogue and take charge of your breast health. There’s more evidence than ever that starting annual mammograms at age 40 saves more lives!